Motherhood is something every woman dreams of experiencing. The first comprehension of life within you, the first movement, the first kick, the first cry of your baby- every moment is as special as the other.
At the same time, pregnancy is also a time when you are susceptible to varied health problems and need proper care. One of these is pregnancy rashes. Generalized skin eruptions encountered during pregnancy can be specific to pregnancy – called specific dermatoses of pregnancy. These can be basically classified into two types:
1. Well-defined rashes: These include herpes gestationis, pruritic urticarial papules and plaques of pregnancy (PUPP) impetigo herpetiformis and recurrent cholestasis of pregnancy.
2. Incompletely defined eruptions: Pruritic folliculitis of pregnancy, prurigo gestationis.
Characteristics of pregnancy rashes:
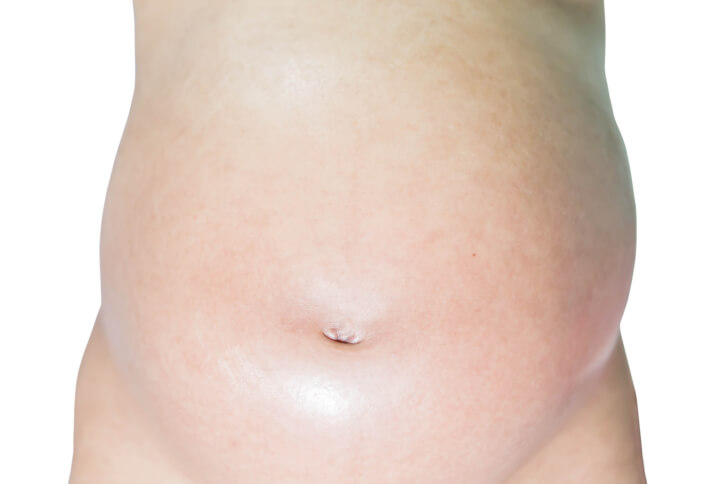
PUPPP: It is one of the commonest pregnancy rashes, found in one out of 130 to 300 pregnant women. A PUPPP related skin rash, characterized by intense pruritus (itching) first appears on the abdomen and is mainly noticed in the third trimester. The skin condition is generally associated with first-time pregnancies.
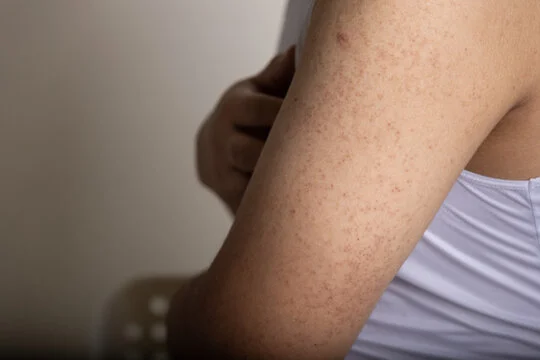
Prurigo: This disorder does not pose any risk to the unborn baby. However, this rash is known to carry on for months after delivery. It is characterized by red bumps, an itchy sensation on arms and legs, and sometimes on other body parts.
Pruritic Folliculitis of Pregnancy: This rash is very common and found on the legs, back, arms and abdomen. It is not risky to the unborn baby and clears out after pregnancy.
Impetigo Herpetiformis: This skin disorder is commonly noticeable in the second trimester. This rash is characterized by sores and releases pus. These are open sores, which can cause infections. It could be highly hazardous for infants and can cause infant deaths.
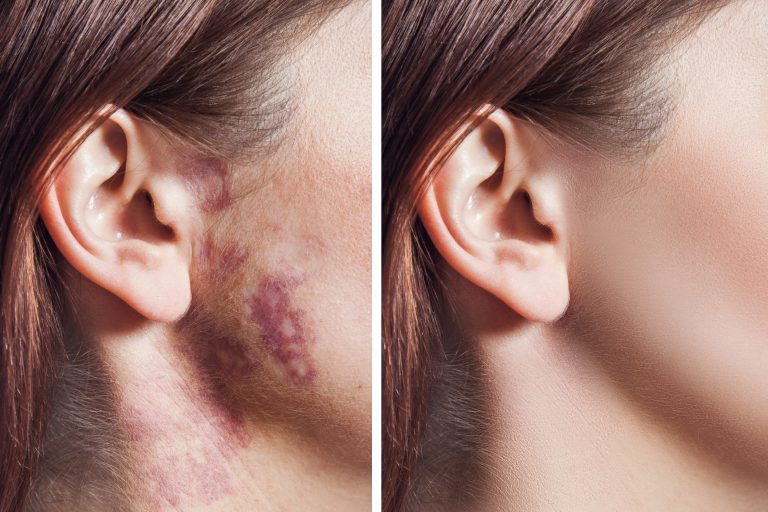
Pemphiogoid Gestationis: This is an uncommon skin rash known to affect one in every fifty thousand pregnancies. This rash is an autoimmune condition characterized by red and brown round-shaped patches on the abdomen. Pemphigoid gestationis rash barely affects a pregnant woman’s scalp, neck, or face. It can lead to low birth weight in babies and put women at a high risk of premature delivery.
Striae Gravidarum: This occurs in up to 90% of pregnant women and is usually found in the third trimester. It appears in purple and pink on the arms, thighs, breasts, buttocks, abdomen, and atrophic lines. It is completely risk-free for the newborn baby. It can disappear after delivery.
Apart from these, non-specific rashes which may be allergic, drug induced or microbial infections can also occur.
Treatment of pregnancy rashes
Appearance of pregnancy rashes should immediately be reported to the doctor. Your doctor may advise the following:
- Topical application of moisturizing creams and emollients
- For serious cases, class 2 corticosteroids creams and ointments can be used. In severe cases oral corticosteroids may be given.
- The doctor may also prescribe anti histamine tablets to soothe the itch.
- Pruritic follicullitis responds well to topical benzoyl peroxide and also has been treated with UV phototherapy
Do-it-yourself solutions
1. Take an ice pack or cold compress and apply on to the affected areas
2. Drink plenty of water i.e. at least 8 to 10 glasses throughout the day to stay hydrated and to keep the skin moisturized and healthy.
3. Wear loose and soft fabric underwear and clothing, preferably cotton, which enables the skin to breathe.
4. Stay away from hot showers as they dehydrate the skin and worsen the itching sensation. Avoid using loofah scrubs or body brushes while bathing.
The above measures are actually useful to prevent skin rashes during pregnancy, but a visit to your gynecologist is a must whenever symptoms appear.