Most people think psoriasis is just a skin condition but it affects more than just your skin. Coping with Psoriasis can be tough as it affects your confidence level and makes you conscious about your looks. Also, most people with psoriasis also experience the symptoms of Psoriatic Arthritis. Though it is not necessary that people who have psoriasis will suffer from Psoriatic Arthritis but the chances are not zero.
This blog will help you understand the link between Psoriasis and Psoriatic Arthritis and how to deal with both the right way.
Understanding Psoriasis and Psoriatic Arthritis
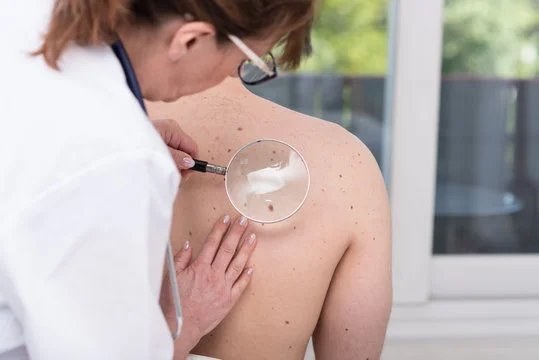
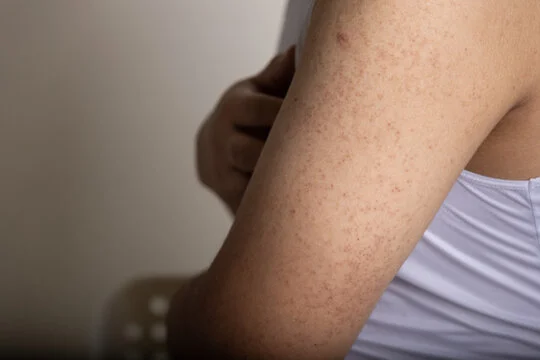
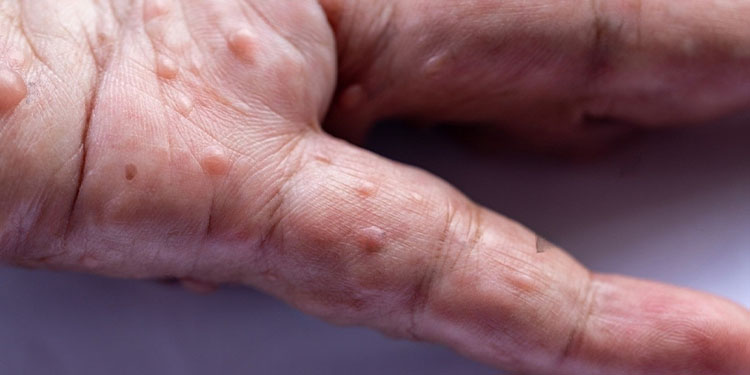
Psoriasis is a condition that manifests as a skin rash and it usually varies in severity over time. It tends to appear on the surface of the skin and can vary from small, pimple-like bumps to large areas of red, splotchy skin. It’s expressed in different ways depending on the patient and how much skin is impacted by its presence has a major impact on the ability of patients to live normal lives.
Psoriatic arthritis (PsA) is a type of inflammatory arthritis associated with psoriasis. People with PsA have joint pain, stiffness and inflammation that can be mild or severe. The symptoms of PsA typically affect the feet, knees and hands but can occur in any joint in the body. Psoriatic Arthritis is a joint condition that is caused by having psoriasis for a long time, usually over 10 years. It affects about 60% of people who have had psoriasis for longer than 10 years.
Causes, triggers and symptoms of psoriasis
The exact cause of psoriasis isn’t known, but it’s thought to be related to your immune system attacking healthy skin cells. The main triggers for psoriasis include:
- Exposure to sunlight
- Stress or anxiety
- Certain foods such as alcohol
- Infections such as colds or flu
Psoriasis causes patches of thickened, scaly skin to appear on the elbows and knees, scalp, lower back and other areas of the body. These patches may be red or purple in colour with silvery scales on top. The severity of psoriasis varies from person to person.
Psoriatic arthritis usually develops after years of having psoriasis but it can develop at any time during someone’s life. Psoriatic Arthritis symptoms include joint pain, swelling on fingers and toes, and inflammation.
The link between Psoriasis & Psoriatic Arthritis
Psoriasis and Psoriatic Arthritis are both autoimmune diseases where your own body attacks healthy tissue. It occurs in around 20% of patients with psoriasis. One commonality between psoriasis and psoriatic arthritis is the chronic inflammation that it causes in a person’s joints, which can actually start the disease process in people who are genetically more prone to it. Besides this similarity, both conditions are genetic.
It is hard to tell whether you’ll experience the skin or arthritis symptoms first which makes diagnosing either condition difficult. However, people who have severe psoriasis are more prone to psoriatic arthritis.
Your doctor will try to gather information about symptoms, any relative who is suffering from this condition or any other autoimmune diseases you’ve suffered from. They’ll also check if you have any pain, tenderness, or swelling in your joints or bones. For further clarity, the doctor will ask you to do some imaging tests like X-rays and MRIs, blood tests, and fluid tests.
Treatment for psoriasis and psoriatic arthritis
Psoriasis and Psoriatic Arthritis treatment is a trial-and-error process. Your doctor will curate a treatment plan for you depending on which of these two conditions is most severe in your case. However, medication for one condition should also have some effect on the other.
There are many medications that can help treat both the skin and joints, but there are definitely medications that work better for one than the other.
Medications use to treat both Psoriasis and Psoriatic Arthritis include:
- Nonsteroidal anti-inflammatory drugs that are used to treat mild joint pain but not skin psoriasis or nail involvement
- Glucocorticoids are used sparingly and very carefully in people with PsA
- Conventional disease-modifying antirheumatic drugs
- Biologics and biosimilars
- JAK inhibitors
Apart from medication, you can also consider making some changes in your lifestyle such as limiting alcohol consumption, exercising daily, maintaining a healthy weight, and managing stress.
The outlook
Both Psoriasis and Psoriatic Arthritis can negatively impact your mental and physical well-being. There is no cure for these conditions but taking medications as prescribed and following doctor’s instructions until it gets better is one sure way to tackle it effectively.
If you are dealing with one or both problems, it is always recommended to consult a doctor to get a clearer picture of your condition. Delaying the treatment will only make things worse. Connect with experts and get more insights on these and other skin conditions at the Skin and Hair Academy.