When your body encounters any offending foreign agent (like viruses, bacteria, or toxic chemicals), it inflames. That’s because the encounter activates the immune system, sending the signal to your white blood cells to fight off the invaders. This makes inflammation a positive indicator that your body’s working as it should. But, while inflammation on the body is expected, such as a bump after a mosquito bite, some flare-ups do more harm than good, just like Stasis Dermatitis.
What is Venous Stasis Dermatitis
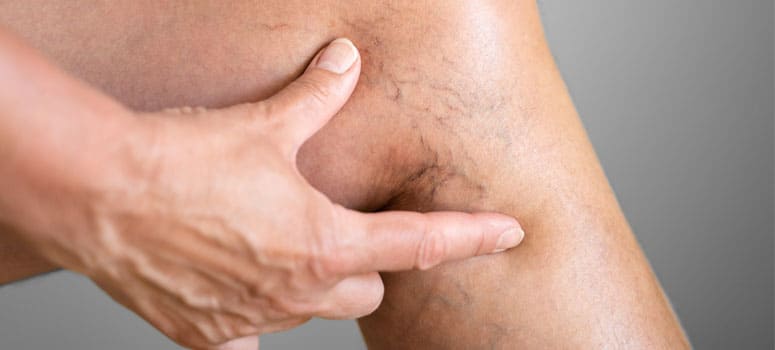
Before we understand this skin condition, how familiar are you with varicose veins? To be on the same page and avoid confusion, varicose veins are defined as enlarged, twisted veins. This can happen to any vein close to the skin’s surface, and these veins commonly appear on the legs. These veins don’t perform the task of blood circulation as they should.
Know that developing varicose veins isn’t an issue that warrants medical attention, apart from cosmetic reasons or when you’ve developed too many of these veins. But sometimes, the story can be different. This brings us back to the topic.
Venous stasis dermatitis is a skin condition involving itchy and swollen discolored skin on the lower legs. The condition often affects people who have blood circulation problems. When the veins don’t work well, they don’t return the blood to the heart like they’re supposed to. To summarize, this is called venous insufficiency, which leads to varicose veins and could trigger venous stasis dermatitis. This skin condition is also known as varicose eczema or simply stasis dermatitis.
Some conditions that make you more likely to get varicose eczema include:
- High blood pressure
- Varicose veins
- Being very overweight
- Heart conditions such as congestive heart failure
- Kidney failure
- A blood clot, especially in your leg
- Many pregnancies
- Past surgery or injury in the area
What are the symptoms of Stasis Dermatitis?
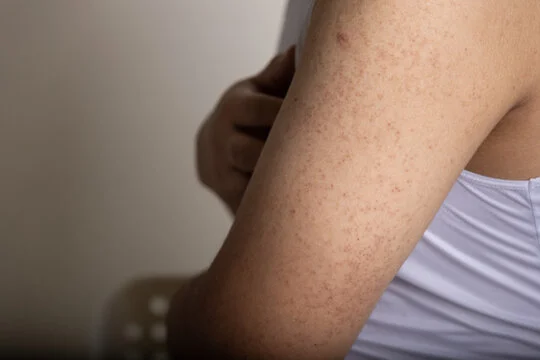
This eczema condition usually affects the feet or the lower parts of the leg. It can be on both sides as well. However, it isn’t limited to just the legs. It can flare up on other parts of the body as well. But this is highly uncommon. Besides ankle swelling, here are other indicators of this skin condition:
- Redness in lighter skin tones
- Brown, purple, or ashen discoloration in darker skin tones
- Patches with intense itching
- Scaling of skin
- Skin dryness
- An achy feeling after long periods of sitting or standing
If stasis dermatitis goes untreated, swelling can move beyond the ankle to the calf and up. Open sores, called venous ulcers, can form on the lower legs and tops of feet. These ulcers can bleed, ooze, and leave scars once healed. This cements the need to get it treated by an expert at the first sign of its appearance.
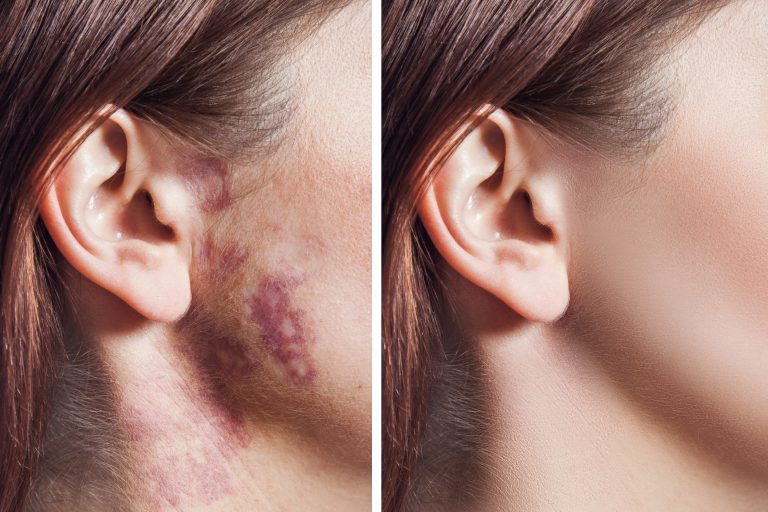
Treatment options for Stasis Dermatitis
This skin condition may look and feel scary. But all is not lost. If given attention by an expert at the right time, controlling isn’t tricky. Stasis dermatitis treatment includes two things, identifying and addressing its root cause as well as managing its symptoms to reduce discomfort. Both physical examinations and blood tests play a role. In short, stasis dermatitis treatment includes:
- Compression stockings to reduce swelling
- Elevating legs above the heart every two hours to reduce swelling
- avoiding foods high in salt
- Supplemental vitamin C and rutin, a plant pigment and antioxidant, to help keep blood vessels flexible and healthy
- For red or darker-colored, itchy skin, dermatologists may prescribe a topical corticosteroid to calm inflammation
- Topical or oral antibiotic if the skin is infected
Conclusion
Stasis Dermatitis, or stasis eczema, is a more common skin condition in people aged 50 or older. Women are more vulnerable to its development than men. But everyone should be aware and conscious of its symptoms. Doing nothing after it has been developed or following unguided home remedies to treat this condition could make it chronic or worse. Severe cases of this skin condition also witness patients developing permanent skin changes, including thickening, hardening, darkening, or a bumpy, cobblestone-like appearance. To avoid that and manage your flares better, consult with a dermatologist to get the proper treatment at the right time.